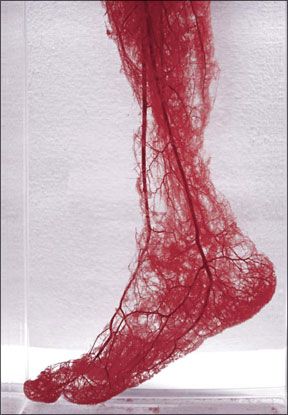
Peripheral arterial disease (PAD) affects about nine million Americans, according to the American Heart Association. In PAD a buildup of plaque in the legs, often occurring in the femoral arteries, can reduce blood flow from the heart to the lower limbs. For most people with PAD, this results in cramping pain in the calf muscles when walking, or in other types of leg pain and decreased function. "However in severe PAD cases, a condition called critical limb ischemia (CLI) can develop," says Heather Gornik, MD, a cardiologist at Cleveland Clinics Robert and Suzanne Tomsich Department of Cardiovascular Medicine. "Sometimes referred to as a leg attack, CLI can be more deleterious to your health than heart attack or stroke."
To continue reading this article or issue you must be a paid subscriber.
Sign in