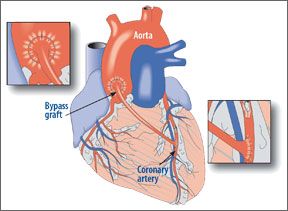
Several criteria must be considered in deciding whether your blocked coronary arteries are treated with bypass surgery or with stents. The size and location of the blockages are perhaps the greatest determining factors, but a recent study suggests that age and diabetes should be part of the equation, too. A study of more than 8,000 heart patients, published in the March 19 issue of The Lancet, found that those patients with coronary artery disease (CAD) who were 65 and older or who were diabetic fared better after bypass surgery than stenting. Cleveland Clinic cardiovascular surgeon Marc Gillinov, MD, suggests, however, that age doesnt significantly raise the risk for either approach. "Both procedures are very safe," Dr. Gillinov says. "Most studies show that patients with diabetes have superior long-term outcomes with bypass surgery if they have three-vessel disease." He adds, however, that three-vessel disease or left main coronary artery disease is typically treated with bypass surgery anyway and that single- or double-vessel disease may be best treated with stents, again depending on all factors. Multi-vessel disease refers to blockages in more than one of the coronary arteries-the blood vessels that supply the heart muscle with oxygen-rich blood.
To continue reading this article or issue you must be a paid subscriber.
Sign in