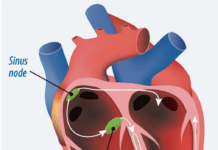
If you have degenerative mitral valve disease, you may want to consider a more aggressive treatment plan than watchful waiting, according to a recent Cleveland Clinic study. Researchers found that earlier surgical interventions, using less-invasive surgical techniques, lead to better outcomes for patients than waiting until some kind of intervention becomes necessary because the condition has advanced to heart failure or atrial fibrillation. Mitral valve disease is the most common type of heart valve problem, affecting about 4 million people in the U.S. Mitral valve regurgitation, in particular, represents the vast majority of mitral valve disorders. Surgery is almost unavoidable in patients with severe degenerative mitral valve regurgitation, says the studys lead author Farhang Yazdchi, MD, formerly of Cleveland Clinic. Our study has shown that the key to successful treatment is a timely referral for surgical intervention at an advanced repair center with highly skilled heart teams. The study was published in the Annals of Thoracic Surgery. If you have mitral valve disease, and are in a watchful waiting mode with your physician, talk with your doctor about the risks and benefits of intervening before the condition worsens. You should also be sure you understand the course your mitral valve disease is likely to follow in the months and years ahead. Remember that you may not notice obvious symptoms of mitral valve regurgitation at first. Eventually, you may notice signs such as palpitations, a cough, shortness of breath, fatigue or lightheadedness. If you feel your condition warrants a more proactive approach, dont hesitate to get a second opinion. The mitral valve is located between the left atrium and the left ventricle, the hearts main pumping chamber.
To continue reading this article or issue you must be a paid subscriber.
Sign in