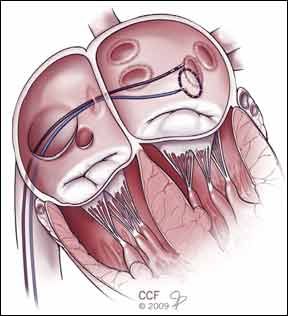
A diagnosis of atrial fibrillation is usually followed by a course of treatment involving antiarrhythmic drugs designed to keep the hearts electrical system under control. Atrial fibrillation (AF) is a condition in which the heart beats abnormally due to erratic electrical impulses originating in the hearts upper chambers, the atria. AF can also be treated with procedures such as radiofrequency ablation, which attempts to destroys the tiny amount of heart tissue that appears to be causing the arrhythmia. Generally, ablation is attempted only after medications prove to be ineffective at controlling AF symptoms.
To continue reading this article or issue you must be a paid subscriber.
Sign in