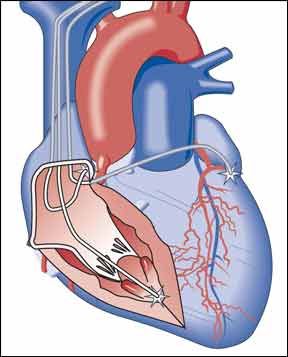
While the number of patients with heart failure (HF) in the U.S. continues to rise, there is some encouraging news on this front. HF-related mortality and hospitalization rates are stabilizing. Improvements in medication and device therapies are helping to make HF a more manageable condition, according to a statement released by the American Heart Association (AHA) in February. The AHA noted that the quality of life for HF patients in general has also improved. Eileen Hsich, MD, director of the Womens Heart Failure Clinic at Cleveland Clinic, has done considerable research in this area, and agrees that many of these vulnerable patients are living longer and better lives because of how and when they are being treated.
To continue reading this article or issue you must be a paid subscriber.
Sign in