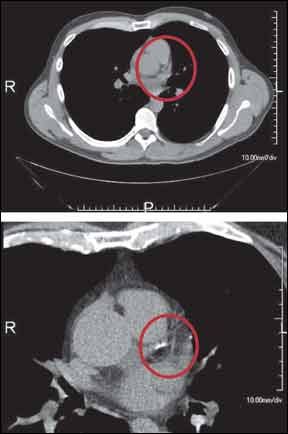
Coronary calcium screenings, in simplest terms, are tests done to give doctors a picture of calcified plaque in your coronary arteries. Plaque build-up can be a risk factor for heart attack and stroke, so evidence of serious calcification could be a helpful predictor of future cardiac events and a red flag to begin or step up treatment. But the issue of calcium screenings is a complicated one. Steven Nissen, MD, chairman of the Robert and Suzzanne Tomsich Department of Cardiovascular Medicine at Cleveland Clinic, believes the screenings are overused and put patients at risk without evidence from large clinical studies that show screening for calcium save lives.
To continue reading this article or issue you must be a paid subscriber.
Sign in