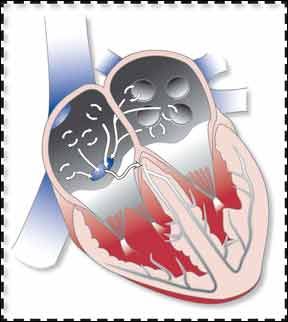
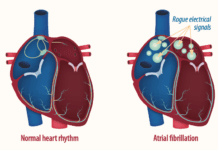
Atrial fibrillation (AFib) is usually characterized by episodes that are noticeable to the patient, who feels a flutter or racing in his heart. But not all arrhythmias are obvious, and a recent study suggests that silent AFib episodes are associated with a 2.5-fold increase in the risk for ischemic stroke. Thats because the chaotic rhythm of a heart in AFib allows blood to pool in the atria (the hearts upper chambers), which can lead to the formation of a blood clot that can break free of the heart, travel to the brain, and block blood flow in an artery, causing an ischemic stroke.
To continue reading this article or issue you must be a paid subscriber.
Sign in